Corneotherapy
Corneotherapy is the link between cosmetics and dermatology on a scientific base.
Corneotherapy is a remedial skin treatment methodology with its core principle being the repair and maintenance of the skin barrier defence systems. As the name suggests, Corneotherapy is closely related to Corneobiology, which is the physiological, biologic and biochemical processes of the stratum corneum; the outermost layer of the epidermis.
It is now widely understood that the outer layer of corneocytes of the stratum corneum is a biologically active cellular tissue. The co-inventor of Retin-A, U.S. dermatologist Dr Albert Kligman and his partners discovered that the stratum corneum, and the lipid barrier that keeps it intact, play a significant role in skin health; it can send many signals to the underlying living epidermis and influences the regenerative processes in deeper layers of the skin.
This understanding of skin health, along with appropriate interventions and topical treatments is an ensemble of therapies that Dr Kligman labelled “Corneotherapy”.
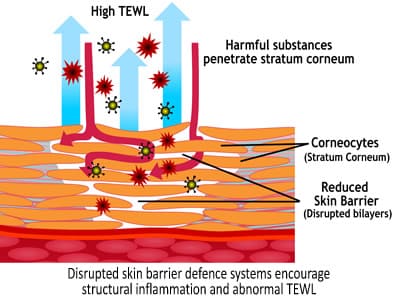
With this knowledge, Corneotherapy centric therapeutic interventions have shown that optimally functioning barrier defences, including a healthy innate immune system can prevent or reduce structural inflammation that is the precursor to many anomalous skin conditions such as EFAD, Xerosis, Itchyosis, and Eczema.
These preventative interventions are primarily directed to correction and restoration of the stratum corneum and barrier defence systems that have been rendered defective or impaired by disease, or intrinsic and extrinsic factors.
The correct application of Corneotherapeutic principles have been shown to restore homeostasis and an improved function of the entire integument; protecting against harmful substances and microorganisms that can trigger these anomalous conditions.
The principles of Corneotherapy can also be applied not just the correction of skin conditions, but for the supportive prevention of skin problems; the prevention of premature skin aging is an inherent outcome of this approach.
A key principle of Corneotherapy is to keep the epidermis intact at all times, with the therapeutic actions working from the outer layers of the epidermis inward. This approach of retaining the integrity of the epidermis ensures the skins defence and immune systems are not stimulated unnecessarily.
Corneotherapy is also an individualized approach to skin care and treatment, following a logical path that investigates and defines the causes of the conditions before selecting appropriate interventions and therapeutic applications in a sequence that achieves the best outcome. This contrasts with the more simplistic approach of treating symptoms without determining the causes.
One of the major advantages of Corneotherapy is that it is largely free of side effects in comparison with a treatment with topical pharmaceuticals. Preventively applied Corneotherapy practices may extend the intervals between flare-ups and reduce or even avoid the application of conventional dermatics such as steroid or cortisone-based creams.
It is these two characteristics:
- taking time to thoroughly investigate the causes of the conditions and
- not just treating the symptoms with repeated application of products with pharmacological action; that perhaps define Corneotherapy from more conventional approaches.
Liposomes
Liposomes are spherical bodies similar to biological cells which are invisible to the naked eye. Like the natural cell membranes of plants and animals, liposomes consist of a so-called bilayer with phosphatidyl-choline as its natural main component. The bilayers of liposomes are very similar to the different layers of the skin barrier, thus liposomes merge easily with those barrier layers. Consequently, the penetration capacity of the skin for cosmetic and dermatologically active substances is improved. Active agents transported inside liposomes penetrate easily and spread well within the skin. They are retained by the skin in a depot-like manner and so often act with stronger effects. Even those active agents that are not encapsulated, but are applied with Liposomes at the same time, are generally more effective.
.jpg)
.jpg)
The following illustrations explain how active agents are transported by liposomes. By merging with the skin barrier layers, the liposomes open up and release the active agents into the skin.
.jpg) Stage 1: A liposome with encapsulated active agents (red) approaches the skin barrier layers.
Stage 1: A liposome with encapsulated active agents (red) approaches the skin barrier layers..jpg) Stage 2: The liposome membrane merges with the barrier layers and opens them. The active agents are released and penetrate through the skin barrier.
Stage 2: The liposome membrane merges with the barrier layers and opens them. The active agents are released and penetrate through the skin barrier.
.jpg) Stage 3: The skin barrier has resealed itself. However, the penetration capacity of the skin is still increased, because of the changed composition of its structure. That is why, in the final step of the treatment, we recommend the application of a DIMS® base cream. It will restore the skin barrier’s natural properties.
Stage 3: The skin barrier has resealed itself. However, the penetration capacity of the skin is still increased, because of the changed composition of its structure. That is why, in the final step of the treatment, we recommend the application of a DIMS® base cream. It will restore the skin barrier’s natural properties.
Nanoparticles merge with the barrier layers in a similar way. In contrast to liposomes that transport aqueous active agents, active agents in nanoparticles need to be liposoluble.
Cosmetic liposomes are always a mixture consisting of unilamellar and oligolamellar liposomes, because the manufacturing process for unilamellar liposomes is more expensive. The lamellarity doesn’t change the encapsulating ability, penetration and efficacy of active agents.
Decisive for the efficacy of liposomes and fluid nanoparticles is only the concentration of phosphatidylcholine (PC). PC does not have its own INCI name, but only appears in the INCI as lecithin, in which it is one component among many others. Lecithin mainly consists of phospholipids with a higher (raw lecithin) or lower (deoiled lecithin) oil content.
Phosphatidylcholine (PC) is a main component of all animal and plant cell membranes and also the intercellular membranes. As a physiological ingredient it is used as a base for the production of liposomes, nanoparticles and DMS® (Derma Membrane Structure). There are two different types:
- PC containing linoleic acid (in liposomes, nanoparticles). The chemically combined linoleic acid is essential and will be released in the skin.
- PC containing palmitic and stearic acid (in DMS8). This PC has ceramide-like properties and is very useful for physiological skin protection. INCI: Hydrogenated Lecithin.
Both types of PC contain chemically bound choline which is essential for the organism but cannot be produced by it. Choline has cell protecting effects.
Nanoparticles
Due to their specific composition, nanoparticles have a high affinity to the horny layer of the skin and are used as transport systems which help the different active agents to penetrate the skin more easily.
Nanoparticles are capsules shaped by a monolayer membrane. This monolayer membrane consists of a substance that is found in the basic structure of cell membranes of every organism in nature. This natural substance has a complex name that is as hard to spell as to pronounce: phosphatidylcholine.
.jpg)
The nucleus of nanoparticles consists of an oily body. Due to its nature, it has the specific capacity of assimilating oil soluble agents like vitamin E, vitamin A, vitamin C palmitate, carotin, the coenzyme Q10, evening primrose oil, wheatgerm oil and shea butter.
Nanoparticles are invisible the naked eyes as well as under the microscope. Only by means of an electron microscope can their structure be revealed. Due to larger particles, the watery dispersion has an opalescent or milky appearance. Speaking of milk: The structure of pure milk is very similar to the structure of nanoparticles, with the difference that the milk particles are larger and that their outer layer, besides phosphatidylcholine, contains other substances like proteins and cholesterol. Also, chylomicrons that transport fats in the blood and lymph stream are related to nanoparticles.
.jpg)
Solid nanoparticles in the pharmaceutical field can have undesired side effects, whereas fluid nanoparticles in cosmetic products are completely safe to use. Fluid nanoparticles cannot penetrate through the skin because they dissolve upon contact with the barrier layers of the stratum corneum from where they release the active agents selectively in molecular form. All components are biologically degradable.